Medical Coding in New Jersey – Accurate & Efficient
TMS Billings ensures every claim is coded precisely, submitted quickly, and monitored closely, with medical coding in New Jersey experts, regional specialty-focused teams, immediate denial work, and transparent pricing.
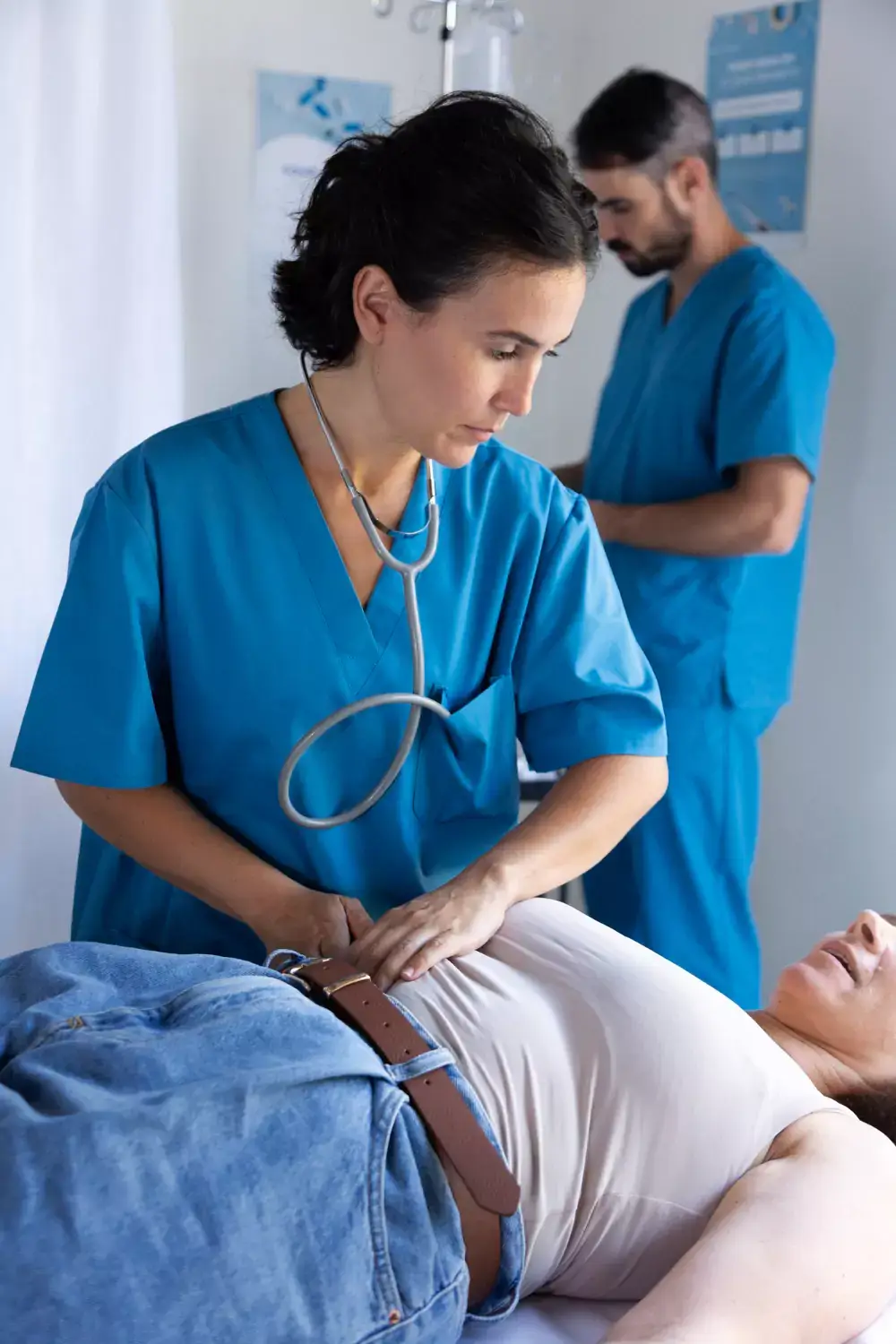


Fast, Accurate Medical Coding to Keep Your Revenue on Track
Tired of billing delays due to coding errors? TMS Billings delivers medical coding in New Jersey with experienced coders who ensure fast payments and keep your revenue on track.
- Medical coding is done accurately to capture all charges, preventing missed revenue and underpayments.
- Claims are submitted within one business day, ensuring quick payment and improving your practice’s cash flow.
- From diagnosis to payer submission, our medical coding services provide clear financial reporting, so you always know where you stand.
- Our medical coding consultants are HIPAA-compliant and stay updated on ICD-10, CPT, and HCPCS codes across specialties.
- At TMS Billings, our coders specialize in fields like mental health, home healthcare, and physical therapy to ensure accurate claims.
Benefits
Achieve Better Cash Flow with Our Medical Coding Services
With our expertise in the latest coding updates, we ensure your claims stay compliant, minimizing audit risks, and avoiding the issue of overcharging patients.
Faster Payment
Claims are submitted within one business day, speeding up the revenue cycle.
Maximize Revenue
We ensure accurate coding to capture every charge, reducing missed payments.
Real-Time Reporting
Get up-to-date financial reports showing claim status, AR, and balances for full transparency.
Tackle Backlogs
We clear coding backlogs quickly and provide regular coding audits for compliance.
Experienced Coders
Our coders specialize in mental health, home healthcare, and physical therapy, ensuring accurate, compliant claims.
How We Handle Medical Coding at TMS Billings
At TMS Billings, we follow a clear process to ensure your claims are coded accurately, quickly, and compliantly. Here’s how we do it, step by step:

Document Review
We start by reviewing the patient’s clinical documentation to ensure we capture every relevant detail for accurate coding.
Analysis and Code Assignment
Our experienced coders analyze the documentation and assign the correct codes based on the patient’s diagnosis and procedures.
Code Verification
Before submitting, we double-check all codes to ensure they align with payer requirements and meet all regulatory standards.
Claims Submission
Once the codes are verified, we submit the claims within one business day, speeding up the reimbursement process.
Quality Assurance
Our coders perform a final review to ensure everything is accurate, compliant, and ready for payment—avoiding errors and rework.
Start a Conversation
you Deserve our best Medical Care



Frequently Asked Questions
Do you have questions about our medical billing and coding company? Let’s help you out.
Do you only work with New York practices?
New York is the core focus. We also support surrounding states when a group has locations that cross state lines, for example New Jersey and Connecticut. The approach stays the same. Regional payor rules, portals, and workflows, not generic billing.
Do you handle New York Medicaid, both fee for service and managed care?
Yes. We handle New York Medicaid fee for service workflows tied to eMedNY, plus Medicaid managed care plan billing. That includes eligibility checks, claim status follow up, denials, resubmissions, and appeals.
What is eMedNY, and why does it matter?
eMedNY is New York’s Medicaid system for provider billing operations, reference material, and tools like claim status inquiry. If a billing team does not know how to work eMedNY correctly, you usually see it in slow claim fixes and aging A R.
We already have a workflow. What changes when we switch?
We merge into your existing workflow. If you want, we take specific steps off your staff’s plate while you keep control of the rest. If you want a full transition, we take the workflow over from the prior billers and keep it moving with minimal disruption.
Will you work inside our current EMR, PM, and clearinghouse?
Yes. Most practices want continuity. We work in your existing system and document the workflow so your team knows what is happening and where to look.
If you do not have a platform, or your current platform is controlled by a billing vendor and you cannot keep it, TMS can provide a platform so you are not boxed in.
If your practice prefers paper and superbills, we can run the workflow that way too.

Stay Up-to-Date with Our Billing Insights

- Billing, Guides
Folks, if you are part of the healthcare world, you’ve likely heard of “laboratory medical billing.” While it may

- Guides
Medical billing is filled with terms that require specific knowledge. You need more than basic information to understand and

- Guides
Submitting accurate claims is just one part of medical billing, but understanding the documents sent by the insurance company
Maximize Payments with Reliable Medical Coding

