If you’re working in the healthcare industry, you’ve probably heard the term HIPAA thrown around quite a bit. But do you know just how important HIPAA compliance in medical billing really is? HIPAA compliance isn’t just a set of rules; it’s a crucial framework to ensure the privacy and security of patient information. And when it comes to medical billing services, staying compliant with HIPAA is essential not only for protecting sensitive data but also for ensuring that your practice avoids costly penalties. But don’t worry, navigating HIPAA compliance doesn’t have to be intimidating. Let’s break it down and make it simple.
What is HIPAA?

Credit: compyl.com
In simple words, HIPAA, or the Health Insurance Portability and Accountability Act, was enacted in 1996 to safeguard the privacy and security of health information. It’s designed to protect patients’ confidential data and ensure that only authorized individuals have access to it. But here’s the thing: as the healthcare industry evolves, so do the challenges in maintaining HIPAA compliance, especially in medical billing.
Why is HIPAA Compliance So Important in Medical Billing?
In the medical billing world, compliance is everything. Imagine your practice dealing with hundreds of patient information records every day. Each one contains sensitive health data. If that data is exposed, not only is your practice at risk of facing HIPAA violations, but it could also harm your reputation and trustworthiness.
HIPAA compliance ensures that the data being handled is protected at every step, from diagnosis to payment. Plus, violations of HIPAA regulations can lead to hefty fines, legal consequences, and even the closure of your practice.
Key Areas of HIPAA Compliance in Medical Billing
The importance of HIPAA compliance in medical billing services cannot be overstated. Properly securing patient data builds trust and prevents costly legal issues. Here’s what you need to know about key areas of HIPAA compliance.
Understanding Protected Health Information (PHI)
The first step in maintaining HIPAA compliance is understanding PHI. This includes any health data that can identify a patient, such as medical records, test results, and even billing processes.
PHI is the heart of HIPAA compliance efforts. In medical billing, PHI is often handled when submitting claims or processing reimbursements, so it’s crucial to ensure that this data is encrypted, secure, and only shared with authorized parties.
Data Security and Encryption
If you’re dealing with medical records or billing information electronically, ensuring that your systems are secure is non-negotiable. HIPAA compliance requires that any electronic data transfers (like emails or e-faxes) be encrypted. This is one area where healthcare organizations need to be vigilant. With cyberattacks becoming more common, encryption isn’t just a “nice-to-have” feature; it’s a requirement.
- Always encrypt electronic transmissions (emails, faxes).
- Use billing software with HIPAA compliance for storing and transmitting patient information securely.
- Ensure your software and systems are regularly updated with the latest HIPAA security rule standards.
Employee Training
HIPAA compliance is not just about technology; it’s about people, too. All employees involved in medical billing services should receive comprehensive employee training on HIPAA requirements.
This training should cover everything from what constitutes PHI to how to handle data securely. Employees need to understand how serious the implications of a data breach are, not just legally but also in terms of trust and patient care.
- What qualifies as PHI and how to handle it.
- The risks of non-compliance and potential HIPAA violations.
- How to securely transmit and store PHI in compliance with HIPAA regulations.
Access Control
You don’t need everyone in the office to have access to all patient data. A strict access control policy ensures that only authorized personnel can access certain sensitive information.
For example, medical billers might only need access to billing codes and diagnosis-related information, not the entire medical history of the patient. Limiting access helps reduce the chance of unintentional data exposure.
- Implement role-based access: Only allow staff access to the data they need to do their jobs.
- Use strong password protocols for accessing electronic records.
- Monitor who accesses sensitive data and when using audit trails to maintain a secure environment.
Audits and Monitoring
One of the most effective ways to ensure ongoing HIPAA compliance is regular audits. You should have systems in place to track access to PHI, monitor suspicious activity, and ensure all electronic transactions are compliant with HIPAA requirements. Regular monitoring allows you to spot potential issues before they become violations.
- Periodic review of user access logs to monitor unauthorized access attempts.
- Conducting regular internal audits to assess security risks in your practice management.
- Monitoring for unusual patterns in data access and flagging for review.
Use of Business Associates
Many healthcare practices work with third-party vendors for medical billing services. These vendors must also comply with HIPAA.
The “Business Associate Agreement” (BAA) is a crucial legal document that ensures the third party will uphold the same standards for confidentiality and security. Without a business associate agreement, you could be held liable for a breach caused by your third-party vendor.
4 Key Regulations of HIPAA

Credit: mailhippo.com
These regulations form the backbone of secure and compliant medical billing practices.
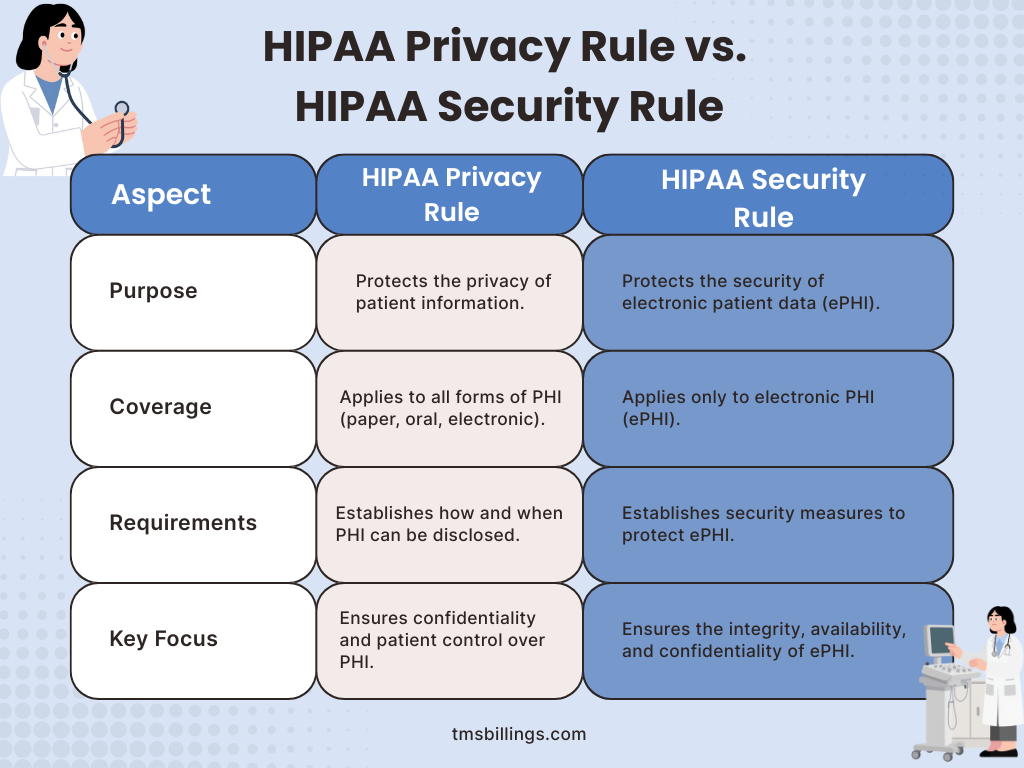
HIPAA Privacy Rule
The Privacy Rule mandates that health information be protected and establishes the conditions under which PHI can be used or disclosed. It ensures that patients have control over their health information, including the right to access and correct their health records.
HIPAA Security Rule
The Security Rule establishes national standards for securing electronic PHI (ePHI). It focuses on safeguarding health information that is electronically stored or transmitted, ensuring that appropriate technical safeguards are in place.
HIPAA Breach Notification Rule
This regulation requires healthcare providers to notify individuals if their protected health information has been compromised. It also mandates the reporting of breaches to the U.S. Department of Health and Human Services (HHS) and, in some cases, to the media.
HIPAA Enforcement Rule
The Enforcement Rule sets civil penalties for non-compliance. It outlines how HIPAA violations are investigated and the penalties that can be imposed. The severity of the penalties depends on the nature and extent of the violation.
How to Maintain HIPAA Compliance in Medical Billing
Now that you know what HIPAA compliance looks like, how can you ensure that your practice stays compliant?
- Adopt Strong Encryption Practices – Always use encryption for storing and transmitting PHI. Whether you’re emailing a claim to an insurance company or uploading medical records to an electronic health record (EHR) system, make sure everything is protected.
- Keep Systems Updated – Cybersecurity threats evolve rapidly. Keep your software, firewalls, and systems up-to-date to defend against potential vulnerabilities and maintain HIPAA compliance.
- Conduct Regular Staff Training – Regular refresher courses on HIPAA compliance for all employees help ensure that your team is aware of the latest standards and practices in handling patient information.
- Data Retention and Disposal Plan – Keep patient data only as long as necessary for billing processes or medical purposes. Once it’s no longer needed, securely dispose of it by shredding paper documents or securely erasing electronic records.
- Establish a Clear Incident Response Plan – In the event of a data breach, having a response plan can help you address the issue quickly. A response plan should include steps to notify affected patients, report the breach to the authorities, and mitigate damage.
Ending Remarks
In a nutshell, HIPAA compliance in medical billing isn’t just a legal requirement; it’s vital for safeguarding patient trust and securing sensitive health information. By understanding PHI (Protected Health Information), implementing data security measures, training staff, and adopting best practices, your practice can not only avoid penalties but also maintain a reputation of reliability and trust.
Frequently Asked Questions
These answers will guide you through the most common queries regarding HIPAA compliance.
What is HIPAA compliance in medical billing?
HIPAA compliance ensures that patient data, including billing information, is protected, stored, and transmitted securely, following the standards set by the HIPAA Act.
Why is HIPAA important in medical billing?
It is crucial because it ensures patient privacy, reduces the risk of data breaches, and helps healthcare organizations avoid heavy fines and legal consequences.
How do I maintain HIPAA compliance in my practice?
To maintain HIPAA compliance, ensure that your systems are secure, encrypt PHI, train your employees regularly, and regularly audit and monitor access to sensitive information.
Can third-party billing companies handle HIPAA-compliant medical billing?
Yes, but they must sign a Business Associate Agreement (BAA) to confirm they will comply with HIPAA standards when handling your patient data.
What are the penalties for HIPAA violations in medical billing?
Violating HIPAA can lead to fines, penalties, and even the closure of your practice. Penalties range from $100 to $50,000 per violation, depending on the severity.