When it comes to medical billing, one of the most crucial parts is Accounts Receivable (AR). If you’re in the healthcare world, you’ve probably heard the term AR in medical billing thrown around, but what does it really mean? Well, think of AR as the process of managing the payments that healthcare providers are owed for the services they’ve already delivered. And let’s be honest—getting paid on time is vital. Effective AR management keeps the cash flowing, prevents financial hiccups, and ensures that practices and hospitals stay financially healthy.
Well, now I’m going to break down everything you need to know about AR in medical billing, how it works, and why it’s so important for keeping your operations running smoothly. Plus, we’ll dive into how AR recovery services and AR follow-up in medical billing can really turn things around when it comes to managing overdue payments. Let’s get started!
What is AR in Medical Billing?
So, first things first. What exactly is AR in the medical billing world? Accounts receivable, also known as medical AR, refers to the process of tracking and collecting payments from patients, insurance companies, and other third-party payers. This process involves managing unpaid claims, following up with insurance companies, and ensuring that healthcare providers get paid for their services.
Key Components of AR in Medical Billing
- Insurance Verification: Confirming that insurance covers the service.
- Claim Submission: Submitting claims to insurance companies for reimbursement.
- AR Follow-up: Checking on unpaid claims and resolving issues with payers.
- Payment Posting: Recording payments from insurance companies and patients.
Understanding AR in healthcare and how it works is crucial for improving revenue cycles and ensuring consistent cash flow. To streamline your AR process, consider utilizing AR recovery services that can help track overdue payments and boost your collections.
The AR Process in Healthcare
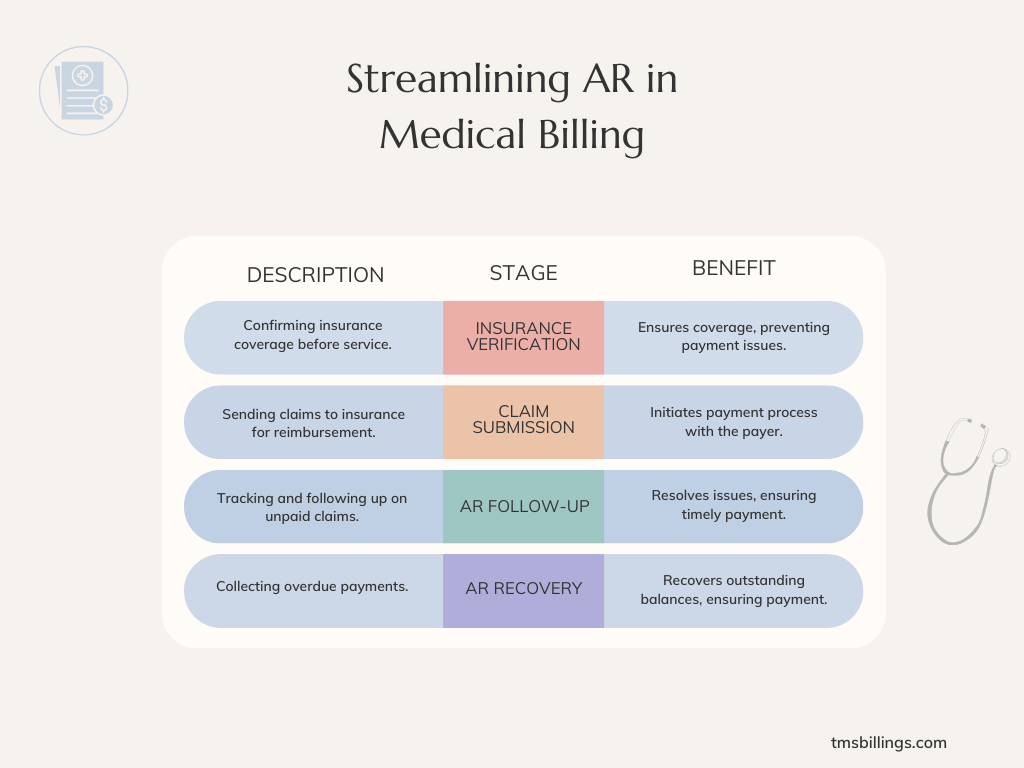
The AR process in healthcare is a multi-step procedure that starts when a patient receives services and ends when the provider gets paid. It includes several stages, from claim submission to AR follow-up, and finally, to recovery.
Stages of the AR Process
- i. Insurance Verification: Before services are provided, verify the patient’s insurance details to ensure coverage.
- ii. Charge Entry: The provider enters charges into the system for the services rendered.
- iii. Claim Submission: Submit the claim to insurance or third-party payers.
- iv. Follow-up and Denial Management: If the claim is denied or unpaid, follow up with the insurance company for clarification or to resubmit claims.
- v. Payment Posting: Once payment is received, it is posted to the patient’s account.
The AR process is crucial for maintaining a healthy revenue cycle and minimizing unpaid claims. If you need help with this process, consider using AR recovery services to speed up collections.
The Role of AR Recovery in Medical Billing
AR recovery in medical billing plays a vital role in ensuring healthcare providers receive payment for services rendered. When claims go unpaid, they accumulate in the system, creating a backlog of revenue. Efficient AR recovery strategies can help clean up these overdue accounts and boost the overall financial health of a practice.
Benefits of AR Recovery
- Faster Payments: Accelerates the collection of overdue payments.
- Improved Cash Flow: Ensures that healthcare providers are paid for the services they provide.
- Reduced Claim Denials: Helps identify issues with claims before they become bigger problems.
- Increased Revenue: Maximizes collections by following up on all outstanding balances.
AR recovery solutions are designed to help medical practices focus on patient care while experts handle the financial side of things.
AR Follow-up in Medical Billing: Why It’s Crucial

Credit: aqkode.com
AR follow-up in is the process of tracking outstanding claims and ensuring that they’re paid. It’s a crucial part of the billing AR process and often requires a lot of time and attention to detail. Without proper follow-up, claims can sit unpaid for months, leaving healthcare providers at risk of revenue loss.
Why AR Follow-up Matters?
- Prevents Delays: Following up ensures that claims aren’t forgotten or delayed.
- Improves Reimbursement Rates: Timely follow-up increases the likelihood of payment.
- Reduces Denials: Regular follow-ups can help identify claim issues early, minimizing denials.
You know, proper AR follow-up in medical billing not only improves the speed of collections but also strengthens relationships with insurance companies by ensuring clear communication.
How AR Recovery Services Improve Your Bottom Line
If your medical practice or healthcare facility is struggling with overdue accounts, AR recovery services are a must. These services are specifically designed to help healthcare providers collect payments faster and more efficiently.
Benefits of Using AR Recovery Services
- Maximized Collections: Helps ensure that every outstanding claim is pursued.
- Dedicated Experts: AR recovery services employ specialists who know how to navigate insurance companies and resolve issues quickly.
- Reduced Administrative Burden: Outsourcing AR recovery allows your staff to focus more on patient care.
If you’re ready to streamline your AR recovery process, consider using professional AR recovery solutions like the ones we offer. Our team can help manage your medical AR efficiently and increase your practice’s cash flow.
FAQ’s
Got questions regarding the AR world in medical billing, let’s answer them!
What is AR in medical billing?
AR in medical billing refers to managing the payments owed to healthcare providers by patients, insurance companies, and other third-party payers. This includes submitting claims, following up on unpaid claims, and ensuring timely payment.
What is the AR process in healthcare?
The AR process in healthcare includes insurance verification, charge entry, claim submission, follow-up on unpaid claims, and payment posting to ensure providers receive reimbursement for services rendered.
How does AR recovery help in medical billing?
AR recovery helps speed up the process of collecting overdue payments by following up with insurance companies and patients, ensuring that no outstanding claims are ignored.
What is AR follow-up in medical billing?
AR follow-up in medical billing refers to the ongoing process of contacting insurance companies and patients to ensure that claims are paid and resolved.
How can AR recovery services benefit healthcare providers?
AR recovery services help healthcare providers collect unpaid claims faster, improving cash flow and minimizing the risk of revenue loss due to unresolved accounts.
Wrapping Up
Summing it all up, AR in medical billing plays a vital role in the financial health of healthcare practices. Whether you’re just starting to manage your accounts receivable or are looking to improve your existing processes, understanding the AR process and utilizing AR recovery service can make a huge difference. By focusing on efficient AR follow-up in medical billing and investing in AR recovery services, healthcare providers can ensure smoother operations and improved revenue cycles.
UP YOUR AR GAME!




